Written by: Precious Eze
Medically Reviewed by: Dr. Deborah Akinlola
Last reviewed: April 11, 2026
Yes, antibiotics can sometimes contribute to bacterial vaginosis, but they don’t cause it in the same direct way they can trigger a yeast infection. Bacterial vaginosis, or BV, happens when the normal balance of bacteria in the vagina shifts and certain bacteria overgrow. The CDC, ACOG, and Cleveland Clinic all explain BV as a bacterial imbalance, not a classic sexually transmitted infection.
This distinction is important. Antibiotics are meant to kill bacteria, but they can also reduce some of the helpful bacteria that help keep the vaginal environment stable. When this balance changes, BV can become more likely in some women.
Click to Jump
What is bacterial vaginosis?
BV is one of the most common vaginal conditions in women of reproductive age. The CDC’s treatment guidance explains that BV develops when protective lactobacilli decrease and other bacteria increase.
Common BV symptoms include:
- thin gray, white, or off-white discharge
- a fishy vaginal odor
- odor that seems stronger after sex
- mild burning or irritation in some cases
Not every woman with BV notices symptoms. Some only notice a change in odor or discharge. Others notice nothing at all.
Can antibiotics lead to BV?
They can contribute, yes. A more accurate way to say it is that antibiotics may disrupt the vaginal microbiome in a way that makes BV more likely in some women.
This doesn’t happen to everyone. Many women take antibiotics and never notice vaginal symptoms. Others develop discharge, odor, itching, or burning during treatment or soon after. Sometimes the cause turns out to be BV. Sometimes it turns out to be yeast. Sometimes it’s irritation or another condition entirely.
This is where the confusion starts. Many women notice symptoms after antibiotics and assume it must be BV, when it may actually be yeast. If that sounds familiar, Can Antibiotics Cause a Yeast Infection? What Women Should Know can help you sort out the difference.
Why antibiotics can affect vaginal balance
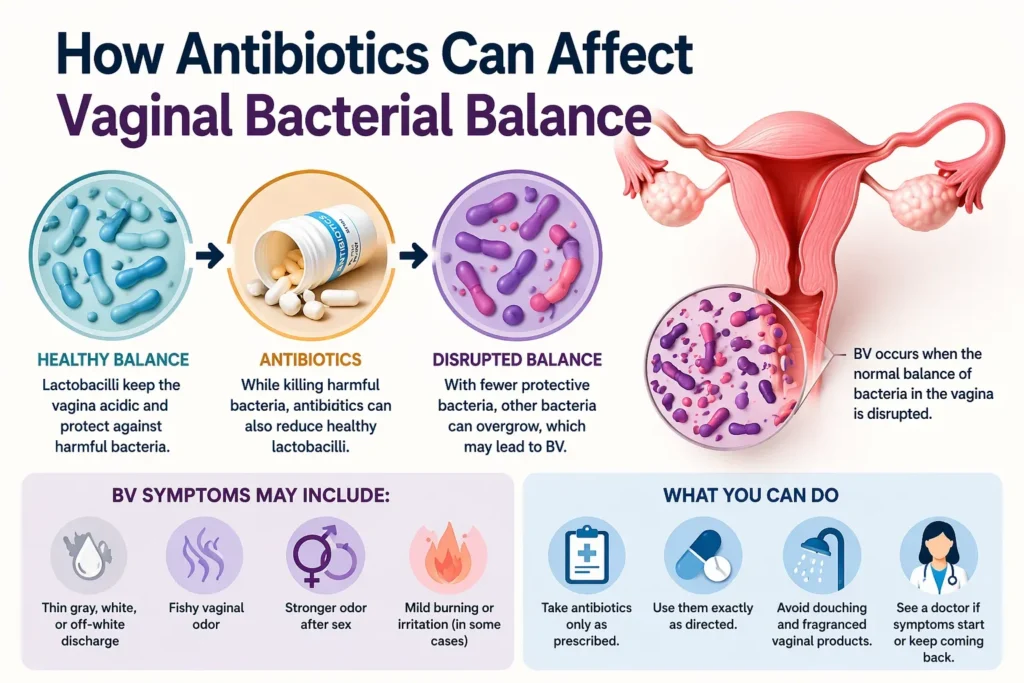
The vagina is healthiest when certain protective bacteria help maintain an acidic environment. When that environment changes, other bacteria can grow more easily. The CDC explains that BV involves a shift away from normal lactobacillus-dominant flora toward other bacteria associated with BV.
This helps explain the link with antibiotics. They are designed to kill bacteria, but they do not always spare the bacteria that help keep the vaginal environment balanced. This does not mean antibiotics always cause BV. It means they can sometimes make the vaginal environment less stable.
This same pattern also explains why symptoms can seem to change after treatment. Sometimes the confusion starts after treatment, when BV symptoms improve but itching or thick discharge shows up next. If that happens, Can Metronidazole Cause a Yeast Infection? explains why.
Does this happen with every antibiotic?
No. Different antibiotics affect the body in different ways, and every woman’s vaginal microbiome is different too. Your risk may depend on the type of antibiotic, how long you take it, your vaginal microbiome before treatment, and whether you already have other BV risk factors.
The Office on Women’s Health lists several known BV risk factors, including douching, new or multiple sex partners, and lack of condom use. It means antibiotics may be part of the story, but they are not always the only factor.
BV after antibiotics or yeast infection after antibiotics?
This is one of the biggest confusion points, so it’s important to look at the signs.
BV is more likely to cause:
- thin gray, white, or off-white discharge
- a fishy smell
- odor that becomes more noticeable after sex
- mild irritation in some cases
A yeast infection is more likely to cause:
- strong itching
- redness or swelling
- thick white discharge
- burning or soreness
The Cleveland Clinic notes that gray discharge with a fishy odor is more suggestive of BV. While ACOG explains that yeast infection, BV, and other forms of vaginitis can overlap enough to make self-diagnosis difficult.
Hormones can muddy the picture too. Antibiotics are not the only medicine that can affect vaginal balance. Some women also start wondering whether hormones could be playing a role, which is where Can Birth Control Cause a Yeast Infection? becomes useful.
Symptoms that should make you think about BV
BV may be more likely if you notice:
- a fishy vaginal smell
- a new thin discharge that looks gray, white, or off-white
- odor that seems worse after sex
- a change in discharge without the heavy itching often seen with yeast
Dryness points in a different direction. If dryness is the main problem rather than odor or discharge, the cause may be something else entirely. Can Antihistamines Cause Vaginal Dryness? explains one possible reason.
How doctors diagnose BV
You can’t diagnose BV reliably by smell or discharge alone. ACOG explains that similar vaginal symptoms can come from different causes, which is why proper diagnosis is important.
A clinician may use your symptoms, a vaginal exam, vaginal pH, and tests on vaginal fluid to confirm the cause. This is so because BV and yeast infections are treated differently. Using the wrong over-the-counter treatment can delay relief and keep symptoms going longer.
How BV is treated
BV is usually treated with prescription antibiotics. The CDC lists recommended treatment options such as oral metronidazole, metronidazole gel, and clindamycin cream.
This can sound confusing at first, but the difference is simple. The problem is not that all antibiotics are harmful. The issue is that different antibiotics affect different bacteria in different ways. Some can disturb balance. Others are used to treat the bacterial overgrowth that defines BV.
What to do if symptoms start during or after antibiotics
If you notice vaginal symptoms during or after antibiotics:
- do not assume it is automatically yeast
- do not keep self-treating without knowing the cause
- pay attention to odor, discharge, itching, and burning
- get checked if symptoms are strong, new, or recurrent
This is especially important during pregnancy. The Office on Women’s Health notes that BV during pregnancy deserves proper medical attention.
Can BV go away on its own?
Symptoms may sometimes improve, but waiting it out is not always the best move, especially if the odor is strong, the discharge is clearly different, or the problem keeps coming back. The CDC also notes that BV is treatable, which is another reason not to keep guessing for too long.
How to lower your risk after antibiotics
You can’t prevent every case, but these steps may help protect vaginal balance:
- take antibiotics only when they are prescribed
- use them exactly as directed
- avoid douching
- avoid fragranced vaginal products that may irritate the area
- get medically evaluated if symptoms keep returning
The Office on Women’s Health specifically warns that douching can raise the risk of BV.
Antibiotics are only one part of the bigger picture. 3 Common Drugs that Affect Your Vagina looks at other medicines that can affect dryness, irritation, discharge, or infection risk.
When to see a doctor
See a healthcare professional if:
- this is your first time having these symptoms
- you notice strong odor or unusual discharge
- you’re pregnant
- you have pelvic pain, fever, or bleeding
- symptoms keep coming back
- over-the-counter yeast treatment did not help
Recurring symptoms are a good reason to stop guessing. BV, yeast, irritation, and some STIs can overlap enough that self-diagnosis is often unreliable.
FAQ
Not in a simple one-step way. But they can disrupt the normal bacterial balance in the vagina, which may make BV more likely in some women.
No. BV is a bacterial imbalance. A yeast infection is caused by yeast overgrowth. They are different conditions and they do not use the same treatment.
Not unless you are sure it’s yeast. Antifungal treatment does not treat BV.
A fishy odor with thin gray, white, or off-white discharge is one of the most common signs.
No. Many women do not. Risk varies from person to person and depends on other factors too.
The bottom line
Antibiotics can sometimes contribute to bacterial vaginosis by disrupting the normal vaginal microbiome, but they’re not the only reason BV happens. If symptoms begin during or after antibiotics, do not assume it must be yeast. Look at the full sign, especially odor and discharge, and get checked if you are not sure.
Medical disclaimer: This article is for education only and isn’t a substitute for medical care. If you have strong vaginal odor, unusual discharge, pelvic pain, fever, bleeding, or symptoms that keep coming back, see a qualified healthcare professional.




