Written by: Abiola Johnson
Medically reviewed by: Dr. Joan Chika
Last reviewed: March 20, 2026
A vaginal yeast infection is a common fungal infection caused by an overgrowth of Candida, usually Candida albicans. It can cause itching, burning, soreness, redness, and a thick white discharge. It’s common, treatable, and usually not caused by poor hygiene or by sitting on a toilet seat. As Mayo Clinic explains, many women will have at least one vaginal yeast infection in their lifetime.
Click to Jump
Quick Answer
A vaginal yeast infection happens when yeast that normally lives in the body grows too much in the vagina. Common symptoms include itching, burning, irritation, soreness, redness, and a thick white discharge that may look like cottage cheese. It’s usually treated with antifungal medicine. But symptoms like discharge, itching, burning, and odor can also happen with other forms of vaginitis, so the CDC advises proper evaluation when the cause is not clear.
What Is a Vaginal Yeast Infection?
A vaginal yeast infection is also called vaginal candidiasis or vulvovaginal candidiasis. It happens when the normal balance of yeast and bacteria in the vagina changes and yeast begins to overgrow. Small amounts of Candida can normally live in the body without causing trouble. Symptoms start when that balance shifts. Mayo Clinic and the CDC both describe it as a common and treatable infection.
Vaginal Yeast Infection Symptoms
Common symptoms include:
- intense itching in and around the vagina
- soreness or irritation
- burning, especially during urination
- pain during sex
- redness or swelling of the vulva
- thick, white discharge that may look like cottage cheese
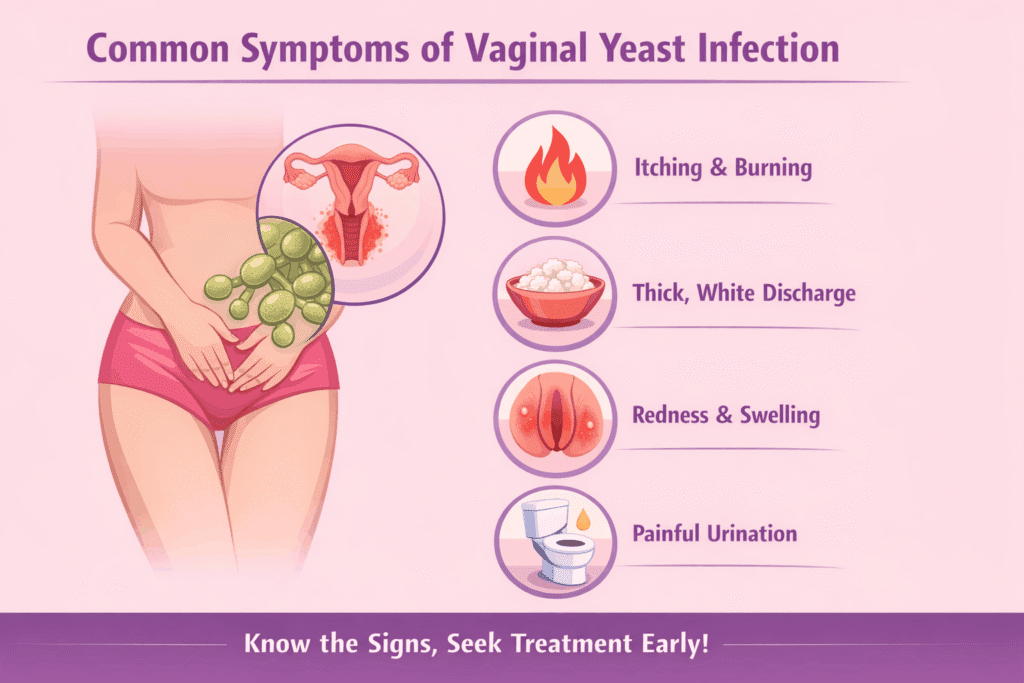
These symptoms can strongly suggest a yeast infection, but they don’t confirm it on their own. The CDC and ACOG both note that vaginal symptoms often overlap. If you’re trying to tell whether the symptoms point more to yeast infection, BV, or an STI, Yeast Infection vs BV vs STI: How to Tell the Difference breaks that down more clearly.
What Causes a Vaginal Yeast Infection?
Several things can raise the risk of yeast overgrowth.
1. Antibiotics
Antibiotics can reduce the helpful bacteria that normally help keep yeast under control. Once that balance changes, yeast can grow more easily, as Mayo Clinic explains.
2. Pregnancy and Hormone Changes
Pregnancy can increase the risk of yeast infection. Hormonal shifts linked to the menstrual cycle or some forms of birth control may also affect vaginal balance in some women. Mayo Clinic also notes that higher estrogen levels can make yeast infections more likely.
3. Diabetes
Poorly controlled diabetes can raise the risk of vaginal yeast infection. Higher blood sugar levels can make yeast overgrowth more likely, according to Mayo Clinic.
4. A Weakened Immune System
When the immune system is weakened, the body may find it harder to keep yeast growth in check. The CDC notes that recurrent or difficult cases may need closer medical assessment.
5. Heat, Moisture, and Irritation
Tight, non-breathable clothing, sweaty underwear, and staying too long in wet clothes can create a warm, damp environment that may encourage irritation and yeast overgrowth. Mayo Clinic includes these among the common risk factors.
Is a Vaginal Yeast Infection an STI?
No. A vaginal yeast infection is not usually classified as a sexually transmitted infection. People who don’t have sex can still get it. But symptoms can still overlap with some STIs and other vaginal infections, which is why ACOG recommends proper evaluation when symptoms are new, severe, or keep coming back.
“Toilet Infection” Is Not the Same Thing
This is one of the most common myths many women hear.
People often use the phrase “toilet infection” to describe itching, discharge, burning, or irritation. But that label is misleading. A vaginal yeast infection is usually linked to an internal imbalance, not to sitting on a toilet seat. Using the wrong label can lead to the wrong treatment, especially when the real problem is BV, trichomoniasis, or another cause of vaginitis.
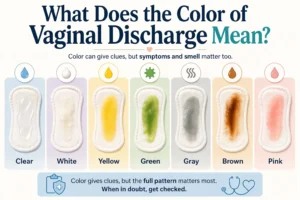
What Vaginal Discharge Can Mean
Many women focus first on discharge, and that makes sense. But discharge alone doesn’t tell the full story. Color, thickness, smell, itching, burning, and irritation all matter. Some discharge is normal, while some patterns point more strongly to infection or imbalance. If discharge is the symptom you’re most worried about, What Causes Vaginal Discharge and When Is It Abnormal? explains what different patterns can mean and when they may need medical attention.
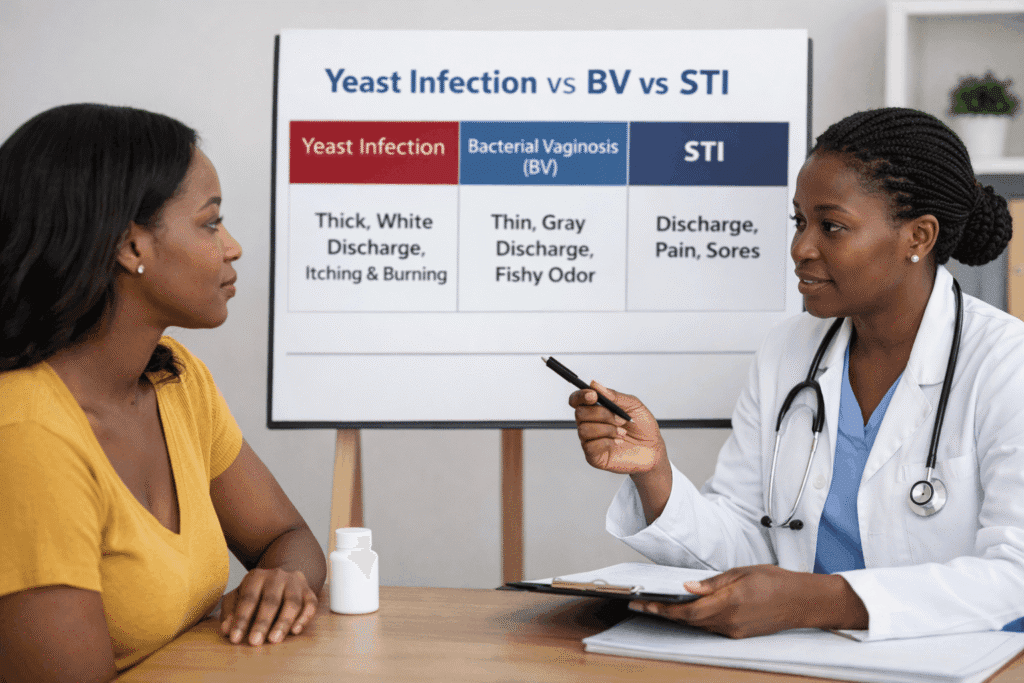
Yeast Infection vs BV vs STI
This is where many women get confused.
A yeast infection more often causes itching, soreness, redness, and thick white discharge. BV is more often linked to a thin discharge and a noticeable fishy smell. Some STIs can also cause discharge, burning, irritation, sores, or pain. The CDC makes it clear that these symptoms can overlap, which is why self-diagnosis is not always reliable.
If the main issue is a strong fishy odor, Why Does My Vagina Smell Fishy? will likely be more useful because that symptom is much more strongly linked with BV than with a typical yeast infection. And if the pattern sounds more like BV overall, Bacterial Vaginosis: Symptoms, Causes, Treatment, and Prevention explains the odor, discharge pattern, causes, and treatment in more detail.
Vaginal Yeast Infection Treatment
Treatment usually works well when the diagnosis is correct. As the CDC explains, treatment commonly includes antifungal medicine such as vaginal creams, suppositories, or an oral antifungal tablet.
Common treatment options include:
- clotrimazole
- miconazole
- terconazole
- fluconazole
The right choice depends on your symptoms, your medical history, whether you are pregnant, and whether this is a first infection or a recurrent one. Mayo Clinic also notes that recurrent or complicated infections may need a different treatment plan.
How Long Does a Vaginal Yeast Infection Last?
With the right treatment, many yeast infections begin to improve within a few days. Full clearing may take longer depending on the treatment used and how severe the infection is. The CDC notes that symptoms should improve with proper treatment. If they don’t improve, come back quickly, or get worse, you should get checked.
Can a Vaginal Yeast Infection Go Away on Its Own?
Some mild cases may improve, but waiting it out isn’t the best plan if you are not sure what is causing the symptoms. The CDC notes that healthcare providers often diagnose vaginal candidiasis by examining a sample of discharge, because symptoms alone don’t always tell the full story.
Recurrent Yeast Infections
If you keep getting symptoms, don’t keep treating yourself blindly. Recurrent infections need proper medical review. They may be linked to diabetes, antibiotic use, immune problems, or another underlying issue. The CDC explains that recurrent vulvovaginal candidiasis needs a different management approach from a simple one-time infection.
Home Remedies for Vaginal Yeast Infection: What to Avoid
Do not put garlic, toothpaste, antiseptics, herbs, or random mixtures inside the vagina. These can irritate delicate tissue and delay proper treatment. ACOG advises avoiding irritants and harsh products in the vulvovaginal area.
Safer supportive steps include:
- keeping the area clean and dry
- washing the outside only with mild soap or plain water
- avoiding douching
- avoiding scented vaginal products
- wearing breathable underwear
These steps may reduce irritation, but they do not cure an active yeast infection on their own.
When to See a Doctor
See a doctor if:
- this is your first suspected yeast infection
- you are pregnant
- you have severe redness, swelling, cracks, or sores
- you have repeated infections
- you have poorly controlled diabetes
- your immune system is weakened
- your symptoms do not improve after treatment
- your symptoms come back quickly
- you are not sure it is actually a yeast infection
These situations may point to a complicated infection or to another condition that needs a different treatment plan. That’s also why Mayo Clinic recommends medical review when symptoms are severe, recurrent, or uncertain.
How to Help Prevent Vaginal Yeast Infection
You can’t prevent every case, but these habits may help reduce the risk.
Wear Breathable Underwear
Cotton underwear can help reduce trapped moisture.
Change Out of Wet Clothes Quickly
Don’t stay too long in sweaty gym wear, wet clothes, or damp underwear.
Avoid Douching
The vagina cleans itself. Douching can upset the normal balance, as ACOG explains.
Avoid Scented Products
Scented sprays, washes, pads, and similar products can irritate the area. ACOG recommends gentle vulvovaginal care.
Manage Blood Sugar
If you have diabetes, good blood sugar control is important.
Get the Right Diagnosis
If symptoms keep coming back, stop guessing. Repeated vaginal symptoms need proper medical review.
FAQ
Usually, no. A vaginal yeast infection is generally caused by an internal imbalance, not by sitting on a toilet seat, as Mayo Clinic explains.
It is often thick, white, and sometimes described as looking like cottage cheese. But discharge alone is not enough to confirm a yeast infection.
Yes. Antibiotics can reduce the helpful bacteria that normally help keep yeast under control.
Some women with a clear history of previous yeast infections may recognize the symptoms, but first-time, severe, or recurrent symptoms should be checked properly.
You usually can’t tell by symptoms alone. Yeast Infection vs BV vs STI: How to Tell the Difference can help you understand the differences, but proper diagnosis still matters when symptoms are new, severe, or recurring.
The Bottom Line
A vaginal yeast infection is common, uncomfortable, and usually treatable. It does not mean you are dirty, and it does not usually come from a toilet seat. But not every itch, burn, or discharge is yeast. The best approach is to know the common symptoms, avoid common myths, get the right treatment, and seek medical advice when the diagnosis is uncertain or the symptoms keep returning.
Medical Disclaimer: This article is for educational and informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always speak with a qualified healthcare professional about personal health concerns.