Written by: Abiola Johnson
Medically reviewed by: Dr. Joan Chika
Last reviewed: March 24, 2026
Not every vaginal symptom means the same thing.
If you have itching, unusual discharge, burning, or odor, the most common possibilities people worry about are a yeast infection, bacterial vaginosis (BV), and sexually transmitted infections (STIs). They can overlap. That’s why self-diagnosis often goes wrong.
Here’s the quick answer:
- Yeast infection is more likely to cause intense itching, irritation, redness, and thick white discharge with little or no odor.
- BV is more likely to cause thin gray or off-white discharge with a strong fishy smell.
- Some STIs are more likely to cause yellow or green discharge, pelvic pain, bleeding after sex, painful urination, sores, or blisters.
Still, symptoms alone don’t always tell the full story. Some women have mixed symptoms. Some STIs cause no obvious symptoms at all. That’s why it’s important to look at the full pattern, not just one sign.
Click to Jump
Quick comparison table: yeast infection vs BV vs STI
| Feature | Yeast Infection | BV | STI |
|---|---|---|---|
| Main clue | Intense itching and irritation | Strong fishy odor | Unusual discharge, pain, sores, bleeding, or exposure risk |
| Discharge | Thick, white, often clumpy | Thin, gray, white, or off-white | May be yellow, green, frothy, or otherwise unusual |
| Odor | Usually little or none | Often strong and fishy | May or may not have odor, depending on the infection |
| Itching | Common and often intense | Mild or absent | Can happen, but not always |
| Burning | Can happen, especially with urination or sex | May happen mildly | Can happen, especially with urination |
| Pelvic pain | Not typical | Not typical | More concerning for an STI or another pelvic problem |
| Sores or blisters | Not typical | Not typical | Can happen with some STIs, such as genital herpes |
| Bleeding after sex | Not typical | Not typical | More concerning for an STI or cervical irritation |
| Best next step | Consider proper diagnosis if it’s unclear or recurrent | Get assessed if odor or discharge suggests BV | Get tested, especially if exposure risk or warning signs are present |
Quick answer: how to tell the difference
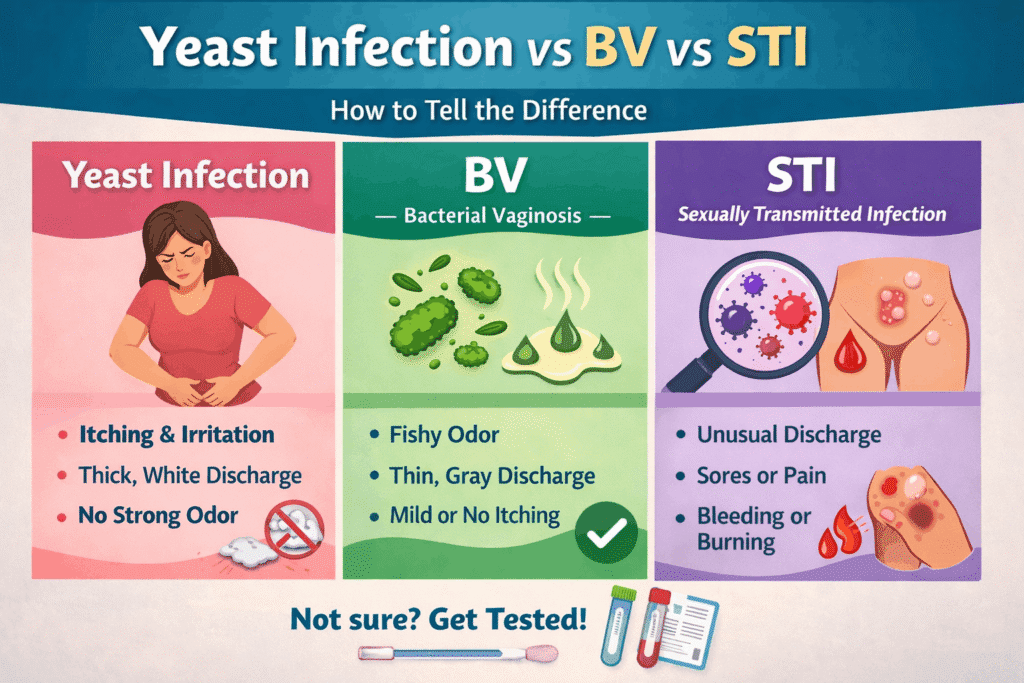
The easiest first clue is usually the symptom pattern.
A yeast infection is more likely if:
- the main symptom is itching
- the vulva feels sore, irritated, swollen, or raw
- the discharge is thick, white, and clumpy
- there’s little or no odor
- sex or urinating causes stinging or burning
BV is more likely if:
- the main change is odor
- the discharge is thin, smooth, and grayish or off-white
- the smell is fishy, especially after sex
- itching is mild or absent
An STI may be more likely if:
- the discharge is yellow, green, frothy, or clearly unusual
- you have pelvic pain
- you bleed between periods or after sex
- urinating is painful
- you have sores, blisters, or ulcers
- you recently had sex with a new partner or had unprotected sex
- your partner has symptoms or has tested positive for an STI
Yeast infection vs BV vs STI at a glance
Yeast infection
A vaginal yeast infection happens when Candida, usually Candida albicans, overgrows. It commonly causes itching, soreness, irritation, burning, and a thick white discharge that may look like cottage cheese. Many women notice little or no strong odor. For a fuller explanation, you can also read our guide to vaginal yeast infection symptoms, causes, and treatment and the CDC guidance on vulvovaginal candidiasis.
Bacterial vaginosis
BV isn’t the same as a yeast infection. It happens when the normal balance of vaginal bacteria shifts. A common clue is a thin gray, white, or sometimes slightly greenish discharge with a fishy smell. Some women also notice mild burning or irritation, but odor is often the biggest sign. This fits with the pattern explained in our article on bacterial vaginosis symptoms, causes, treatment, and prevention and guidance from the NHS.
STI
“STI” is a broad category, so symptoms vary. Some infections can cause discharge, burning when urinating, pelvic pain, bleeding after sex, or genital sores. For example, trichomoniasis can cause yellow-green or frothy discharge, while herpes is more associated with painful blisters or sores. Chlamydia and gonorrhea may cause unusual discharge, pelvic pain, or bleeding, but they can also be silent. The CDC vaginal discharge guidance and ACOG’s vaginitis overview both make it clear that symptoms can overlap.
What the discharge may mean
Discharge is one of the biggest clues, but it isn’t enough on its own.
Thick white discharge
A thick white discharge, especially if it looks clumpy or curd-like, points more toward a yeast infection than BV. That becomes even more likely if there’s strong itching and no fishy smell.
Thin gray or off-white discharge
A thin, smooth discharge with a fishy smell points more toward BV.
Yellow, green, or frothy discharge
That raises more concern for an STI such as trichomoniasis.
Discharge with blood, pelvic pain, or sores
That isn’t typical of a simple yeast infection. It needs proper assessment, especially if you also have lower abdominal pain, fever, bleeding after sex, or painful genital sores.
Itching, smell, and pain: the pattern matters
When women try to self-diagnose, they often focus only on discharge. That’s a mistake. The full pattern matters more.
If the main problem is itching
Think more about yeast infection.
Yeast infections usually cause more itching, redness, swelling, and soreness around the vulva. The irritation can be intense. Burning may happen during sex or when urine touches inflamed skin.
If the main problem is smell
Think more about BV.
A strong fishy smell, especially after sex, is a classic BV clue.
If the main problem is pelvic pain, bleeding, or sores
Think beyond yeast infection and BV.
Pain deep in the pelvis, bleeding after sex, bleeding between periods, or sores and blisters are stronger warning signs for an STI or another gynecologic issue.
Why self-diagnosis often goes wrong
This is where many women get stuck.
They feel itching and assume it’s yeast. Or they notice a strong odor and assume it’s BV. Or they panic and assume every unusual symptom means an STI. Sometimes they buy antifungal medicine straight away, even when the real problem is something else.
That happens because these conditions can overlap. The CDC notes that symptoms like discharge, itching, burning, and odor can appear across different vaginal infections, so symptoms alone aren’t always specific enough to confirm the cause.
A few common self-diagnosis mistakes include:
- treating every itching episode as yeast infection
- assuming odor automatically means an STI
- ignoring exposure risk because the symptoms seem mild
- repeating over-the-counter treatment without getting tested
- focusing only on discharge and ignoring pain, bleeding, sores, or timing
Why recurrent “yeast infection” isn’t always yeast
This is an important point many people miss.
If symptoms keep coming back, it doesn’t always mean you have stubborn yeast. It may mean:
- the original diagnosis was wrong
- the infection was only partly treated
- BV is actually the problem
- an STI hasn’t been ruled out
- there’s irritation from soaps, products, or another non-infectious cause
That’s one reason repeated self-treatment can backfire. If you keep treating “yeast infection” but the real problem is BV or an STI, the condition may continue, worsen, or keep coming back.
Can symptoms overlap or happen at the same time?
Yes, they can.
Real life doesn’t always follow neat textbook lines. Some women have symptoms that blur together. A person may notice itching plus odor. Someone else may have unusual discharge but no pain. In some cases, more than one issue may be present at the same time.
That’s why a symptom checklist is useful, but it isn’t a perfect diagnosis. If the pattern is mixed, recurrent, severe, or just doesn’t clearly fit, testing is safer than guessing.
Can antibiotics or other drugs trigger similar symptoms?
Yes.
Some medicines can upset the normal vaginal balance and make yeast overgrowth more likely. That’s one reason our article on common drugs that affect your vagina is an important companion to this one. If symptoms started after a course of antibiotics, yeast infection may move higher on the list, but it still shouldn’t be assumed automatically.
When it may be a yeast infection
A yeast infection becomes more likely when:
- itching is intense
- the vulva feels raw, red, or swollen
- discharge is thick, white, and clumpy
- there’s little or no bad smell
- symptoms started after antibiotics, pregnancy-related changes, or other shifts that can affect vaginal balance
Still, symptoms alone aren’t perfect. Even the CDC notes that none of the common symptoms is specific to yeast infection by itself.
When it may be BV
BV becomes more likely when:
- discharge is thin and smooth
- there’s a fishy smell
- the odor is more noticeable after sex
- itching isn’t the main complaint
BV isn’t usually classified as an STI, but sexual activity is linked to it, and BV can increase the risk of getting an STI.
When it may be an STI
Think more seriously about an STI if:
- you had unprotected sex
- you have a new sexual partner
- your partner has symptoms
- the discharge is yellow, green, or frothy
- you bleed after sex
- you have pelvic pain
- you have sores, blisters, or ulcers
- symptoms keep returning
- you feel unwell or have fever
Some STIs can be silent, so no symptom pattern rules them out completely.
Red flags you shouldn’t ignore
Get checked as soon as possible if you have:
- pelvic or lower abdominal pain
- fever
- bleeding after sex
- bleeding between periods
- painful sores, blisters, or ulcers
- symptoms during pregnancy
- persistent symptoms that don’t improve
- symptoms that keep coming back
- a new sexual partner plus unusual discharge or pain
These signs don’t always mean something serious, but they do mean self-diagnosis is less reliable.
How doctors tell the difference
Doctors don’t rely on guesswork alone.
Depending on your symptoms, they may use:
- a symptom history
- a pelvic exam
- a vaginal swab
- pH testing
- microscopy or lab testing
- STI testing with approved methods
This matters because the right treatment depends on the right diagnosis. BV is treated differently from yeast infection. STIs also need specific testing and treatment, and some can lead to serious complications if they’re missed.
Don’t treat every vaginal symptom the same way
This is one of the most important takeaways.
Antifungal medicine may help a true yeast infection. It won’t treat BV. It won’t treat chlamydia, gonorrhea, herpes, or trichomoniasis.
So if you’re not sure what’s going on, especially if the symptom pattern doesn’t clearly fit a yeast infection, it’s better to get tested than to keep guessing. That’s especially true if symptoms return, odor is strong, there’s pelvic pain, or there are sores or bleeding.
When to see a doctor

Seek medical care if:
- this is your first episode of unusual vaginal symptoms
- you’re not sure whether it’s yeast infection, BV, or an STI
- symptoms keep coming back
- you’re pregnant
- you have pelvic pain
- you have fever
- you bleed after sex or between periods
- you have sores, blisters, or ulcers
- your symptoms don’t improve after treatment
- you think you may have been exposed to an STI
These are situations where self-diagnosis is much less reliable and missing the right diagnosis carries more risk.
How to lower your risk
You can’t prevent every vaginal problem, but you can reduce avoidable triggers.
Helpful steps include:
- avoid douching
- don’t use random vaginal products unless advised
- practice safer sex
- get tested when needed
- complete prescribed treatment properly
- avoid repeatedly self-treating the wrong condition
- pay attention to symptom patterns after antibiotics or other medication changes
FAQ
Usually, yeast infection is linked more with itching and thick white discharge than with a strong fishy odor. A strong fishy smell points more toward BV than yeast infection.
No. BV isn’t usually classified as an STI, but sexual activity is linked to it, and BV can increase the risk of getting an STI.
Yes. Some STIs can cause irritation, burning, and abnormal discharge, which is why symptoms alone aren’t always enough to tell the difference.
No. It can point toward yeast infection, especially with itching and little odor, but symptoms can still overlap. Persistent or unclear symptoms need proper evaluation.
Sometimes you may suspect the cause from the pattern, but home guessing isn’t always reliable. That’s especially true if the symptoms are new, recurrent, severe, or mixed.
What to Remember
A yeast infection, BV, and some STIs can feel similar at first. But the details often point in different directions.
If itching and thick white discharge are the main problem, yeast infection becomes more likely.
If the discharge is thin and there’s a fishy smell, BV moves higher on the list.
If there’s yellow or green discharge, bleeding, pelvic pain, sores, or a clear sexual exposure risk, think more seriously about an STI.
The safest rule is simple: don’t assume every vaginal symptom is a yeast infection. If the pattern is unclear, keeps coming back, or includes warning signs, proper testing is the better next step.
Medical Disclaimer: This article is for educational and informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always speak with a qualified healthcare professional about personal health concerns.




